Genotyping of the patient's partner was attempted at this time but could not be performed, as his serum viral load remained undetectable. Precore and basic core promoter mutations were not found. By his second visit on May 4, 2006, his aminotransferases had started to trend down and his HBV genotype was found to be type A without resistance to polymerase inhibitors. Laboratory findings were otherwise significant for AST of 1,010 IU/L, ALT of 2,423 IU/L and bilirubin within normal limits. His hepatitis serologies were unchanged, and his HBV DNA level measured 58,900,000 IU/mL. On physical examination, our patient was anicteric and revealed borderline hepatomegaly.  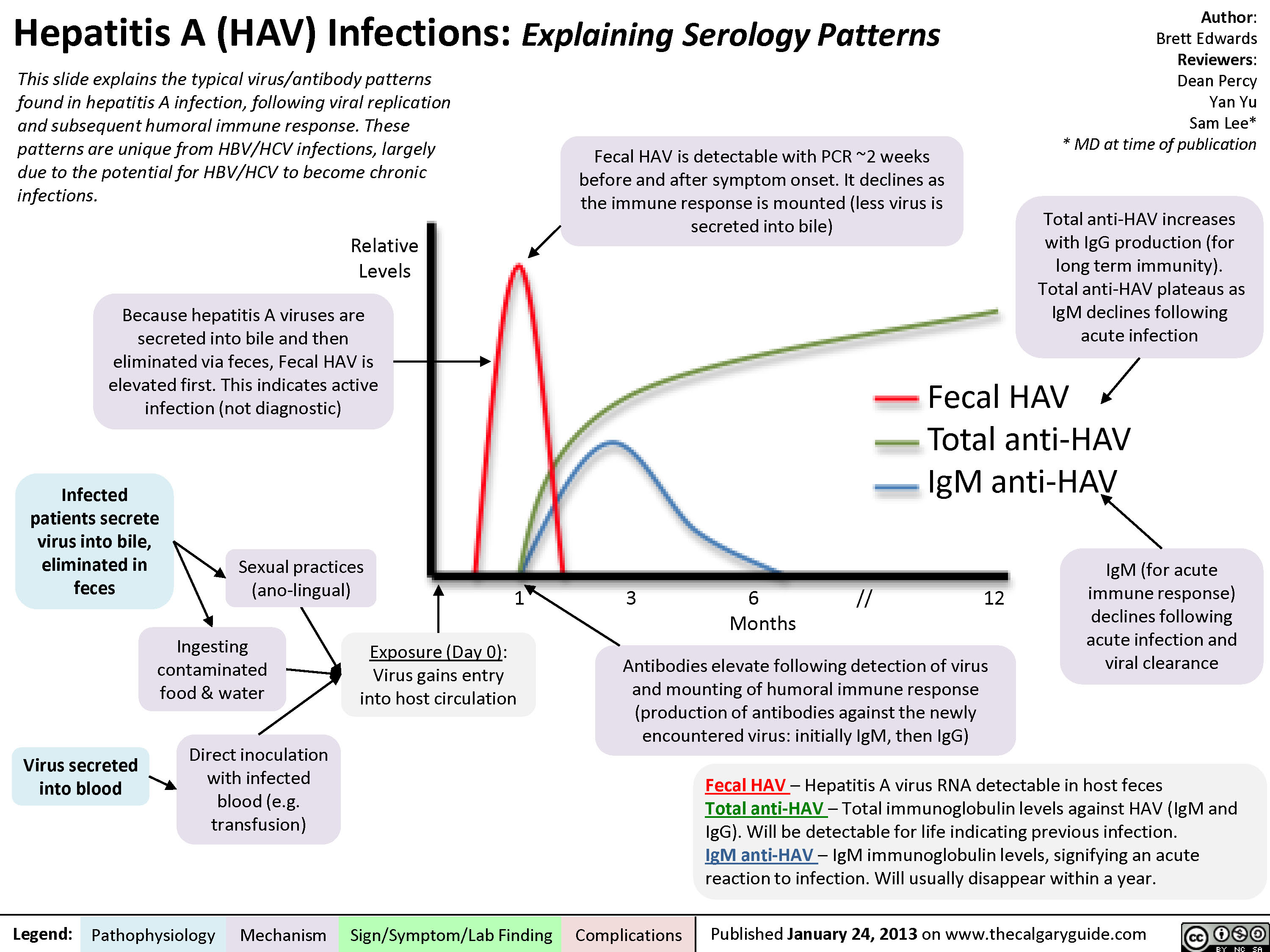
Although the time course from condom breakage to initial presentation of symptoms was consistent with the incubation time of acute HBV, his partner had a documented undetectable serum viral load at that time (6/05: HBV DNA <100 IU/mL, HBeAg nonreactive, HBeAb reactive 11/05: HBV DNA <100 IU/mL, HBeAg nonreactive, HBeAb nonreactive). He otherwise reported adherence to safe sex practices with his partner and denied having sex outside of the relationship. During the initial evaluation, the patient recalled a discrete incident of condom breakage during anal receptive intercourse with his partner in August 2005. The patient was treated with hydroxyzine (Vistaril, Pfizer) and cholestyramine (Questran, Bristol-Myers Squibb) for symptomatic relief.Īt the beginning of May 2006, the patient presented with recurrent symptoms to The Mount Sinai Faculty Practice Associates, where his partner was being followed and treated for chronic HBV with adefovir (Hepsera, Gilead) and lamivudine (Epivir, GlaxoSmithKline). Repeat laboratory examinations 1 week and 1 month later demonstrated worsening transaminitis (AST of 1,400 IU/L rising to 1,625 IU/L and ALT of 1,970 IU/L rising to 2,111 IU/L). His hepatitis serologies tested hepatitis A antibody immunoglobulin (Ig)M-negative, hepatitis B surface antigen (HBsAg)-positive, hepatitis B core antibody (HBcAb)-positive, a hepatitis B surface antibody (HBsAb) level of less than 3.0 mIU/mL, HBeAg-positive, and hepatitis C virus antibody-negative, all of which are consistent with acute hepatitis B infection. His limited physical examination was significant for scleral icterus, and his laboratory work-up at that time was significant for transaminitis (aspartate aminotransferase of 1,081 IU/L, alanine aminotransferase of 1,831 IU/L), hyperbilirubinemia (total bilirubin of 8.6 mg/dL), as well as alkaline phosphatase of 283 IU/L, lactate dehydrogenase of348 IU/L, and gamma glutamyl transferase of375 IU/L. The patient had initially presented to his primary care physician in Texas in November of 2005 for symptoms of jaundice, pruritus, fever, and joint pain. He recalled a prior HBV vaccination in 2000. A homosexual male in a monogamous relationship with his partner, he denied any history of occupational exposure or blood transfusion. The case we present challenges the accuracy of this principle.Ī 37-year-old man from Texas living in New York City was referred to our liver clinic for management of HBV. Patients treated with interferon and/or antivi-rals with adequate response, as demonstrated by hepatitis B e antibody (HBeAb)-seroconversion and undetectable serum HBV DNA levels, are generally accepted to be no longer infective to others. 5 It is recommended that spouses and steady sex partners of those with chronic HBV be vaccinated and follow safe sex practices to prevent sexual transmission of the disease. 4 The risk of HBV transmission from those chronically infected is thought to be highest among those who are hepatitis B e antigen (HBeAg)-positive and those with elevated HBV DNA levels. 3 Although the risk of chronic HBV infection after acute exposure is only 1–5% when infection occurs in adulthood, approximately 1.2 million individuals have chronic HBV in the United States and are sources of infection to others. Sexual transmission is the major mode of transmission in developed countries and accounts for more than 50% of acute HBV infection in the United States. 2 The most common risk factors for HBV infection include injection drug use, sex with multiple partners, and men having sex with men. 1 However, the incidence of HBV among adults has increased since 1999. 
This was the consequence of both a decrease in incidence among homosexual men (from 20% to 7%) due to safe sex education for HIV transmission, as well as a decrease in incidence among children and adolescents (from 8.5 cases to 2.1 cases per 100,000 people) due to the initiation of the HBV vaccination in 1991. The incidence of acute hepatitis B virus (HBV) saw a decline throughout the 1980s and early 1990s.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
